| VARICOCELE |
| ANDROLOGY : The Science of Dysfunctions of the Male Reproductive System |
 | |
| Sex is Not a Four-Letter Word | |
| Publisher: Rupa & Co., India | |
| A sex edutainment book by Dr. Sudhakar Krishnamurti... |
|
| Check with a good bookstore near you! | |
| Buy Online at | |
| • | Rediff Books  |
| • | Google.com |
| • | Amazon.com |
| • | NDTV Fabmall |
| • | Linux Bazar |
| A G A S S I 'Ageing, Gender, Andrology, & Sexual (Sciences), Society of India' |
|
 Impotence often comes without warning and can strike even the most virile stud like a bolt of lightning. How much of a risk do you face ? |
 Sex is man's second strongest instinct. An instinct that is second only to the survival instinct. This means that if a man's life is not immediately imperilled, the next thing he will automatically think of is sex. from WHAT EVERY ADULT NEEDS TO KNOW ABOUT IMPOTENCE |
The vacuum device is an external, non-invasive treatment option for impotence.
This device is available for purchase through this site.
Please Contact Us
More Information on non-invasive treatment options. More Details
 Before the advent of andrology, it was both thought and taught that impotence was psychological in origin. Epoch-making andrologic research in the past decade has shattered this myth and today it is known that in 80-90% of such cases, there is a physical (organic) cause rather than a purely psychological (functional) one. from THE SCIENCE OF ANDROLOGY |
 We've all heard of the barren wife. But what of barren husbands ? Can male infertility be cured ? The wife visits her gynecologist...so who is the husband supposed to consult ? find out in THE MALE FACTOR IN INFERTILITY |
|
The terms 'varicocoele' and 'varicocele' mean the same thing. The first is the British* spelling, and the second's the American one. There are already many other content-heavy varicocele sites out there in cyberspace. Many of these are comprehensive sources of information to medical professionals, varicocele afflicted patients, and lay surfers.
This site doesn't intend to be another such. It is a very basic varicocele information site that's been created especially for men and boys with varicoceles and will restrict itself to practical FAQs that these males or those interested in these males might want answers for. It also provides links to other men's health and andrological conditions, Andromeda Andrology Center, and Dr. Sudhakar Krishnamurti, who is the first Indian infertility microsurgeon to perform microsurgical varicocelectomy surgery (since 1988).
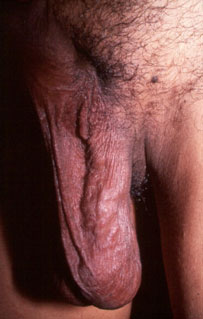
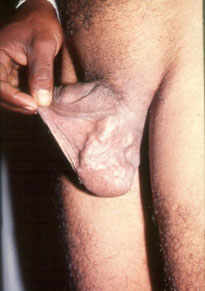
What is a varicocele?
Half of all infertility (50 %) is male partner related, and a varicocele is often the culprit.
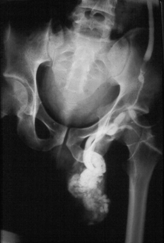
A varicocele frequently presents as a visible swelling in the scrotum, and the scrotum itself may hang lower than usual. Damage to the testis, with reduction in size and function, can sometimes occur. Often, there is a dull, dragging pain accompanying this condition. Frequently, however, the varicocele is not prominent, and may be completely asymptomatic, i.e. without symptoms. It is only discovered incidentally during a male infertility evaluation. varicoceles occur more frequently on the left side and are somewhat more common in lean, tall males.
The varicocele is the commonest treatable cause of male infertility.
What about varicoceles in adolescents? Is this something to worry about?
The adolescent varicocele has been studied quite well over the years. Many of these disappear with age and do not cause any problems in later life. Infertility is uncommon. However, regular examination of the boys until the disappearance of the varicoceles is recommended. Only persisting varicoceles and those causing complications like reduction in testis size must be treated.
Why do varicoceles occur?
Are all men with varicoceles infertile?
About 35-40 % of all men with varicoceles will be infertile as a direct consequence of the varicocele.
What about diagnosis? Is it very difficult?
How about tests? Are they necessary to confirm the diagnosis?
What about treatment? Does it work? There seem to be many opposing views on this.
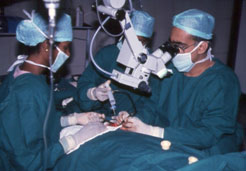
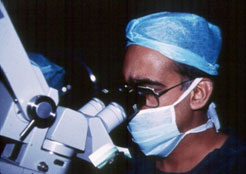
Microsurgery for varicoceles requires microsurgical training for surgeons, assistants, and staff, special operation theatre infrastructure, and instrumentation. The use of optical loupes (magnifying spectacles) is not microsurgery. Microsurgery requires a special operating microscope (see Figure 5). All urologists, andrologists and other surgeons offering surgery for varicocele are not trained microsurgically. Varicoceles can be operated upon even without a microscope, like it was done in the past, but the results are just not as good as those obtained with microsurgery that is performed by skilled microsurgeons with great experience.
Microsurgery allows selective ligation of the veins and avoids injury to the testicular artery and lymphatic channels in the spermatic cord, thus preventing post-operative complications such as testicular damage, atrophy, azoospermia, hydrocele formation, etc.. Recurrence rates with microsurgery are very low too.
Other operative approaches, including laparoscopic varicocelectomy, are much less effective than microsurgery, and carry significantly higher complication rates.
Will patients require IVF (in vitro fertilization) or other ART (Assisted Reproductive Technologies) after varicocele treatment? Or is it better to avoid varicocele surgery altogether and go in for these procedures
instead?
However, the reason why many men with varicoceles are not offered varicocele microsurgery as an option at all, and are persuaded instead to undergo assisted reproductive technologies (ART) like IUI (intra-uterine insemination), IVF (in vitro fertilization) or ICSI (Intra-Cytoplasmic Sperm Injection), is that many of these men have landed up at infertility clinics where the doctors and staff are only trained in such therapies. Most infertility centers do not have an andrologist or uroandrologist on their staff, and often, the man is not even examined physically. He is only asked to furnish samples of semen on the dates his partner ovulates. It is in the interest of these centers to malign varicocele surgery and persuade the patient to undergo other treatments instead. Also, some of these centers see patients who have failed varicocele surgery performed by regular surgeons, and therefore think that it doesn't work. It must be noted that the high success rates boasted with many assisted technologies at infertility centers is a cumulative success rate after many attempts, and that the success rate per attempt (all technologies across infertile women of all ages combined) is hardly ever greater than ten to twenty per cent at most of these centers. The other point to note here is that if a varicocele operation is performed at a center of microsurgical excellence, the man is able to father many children naturally thereafter (see Figure 2) and usually will not need any further medical assistance whatsoever. By contrast, if the first pregnancy in a varicocele patient has been achieved by treating his semen sample and his partner, rather than by treating his varicocele, these torturous ART processes have to be repeated every time the man wants to father a child, until a pregnancy ensues. Each 'cycle' requires the woman to take medicines and injections to induce ovulation (egg release) for several days mid-cycle each month. The lady is also subjected to serial ultrasound scans to confirm ovulation. And then, of course, there are the pokes to pick up the ova (eggs) and all that. Many of these women are working women and some have to travel to the bigger towns to undergo all this. Not too many doctors explain all this to the patient.
Also, it must not be forgotten that the treatment of a varicocele is not for fertility alone. The varicocele is already harming the testis in an infertile male. If only the semen sample is treated, and not the varicocele, this damage continues and the testicular damage becomes worse. Over time, sperm counts may decline dangerously, and testosterone levels may drop, causing additional problems. Also, on the whole, ARTs like IVF and ICSI (Intra-Cytoplasmic Sperm Injection) carry much higher costs than varicocele microsurgery.
The surfer must beware of the websites/ specialists that do not address these aspects, and engage instead only in false propaganda that suits their interests more than the patients'.
Lastly but importantly, in male dominated societies, it is common for men to shy away from treatment for their own infertility. Instead, they persuade the partner to seek treatment. This is unfair, unscientific, and, as has been discussed above, is not in the best interests of the couple.
To summarize, it may be quite accurate to state here that if, in an infertile couple, there is a varicocele male factor that is impairing semen quality and causing infertility, that varicocele must be treated microsurgically at a center of excellence. This is especially important if the woman is normal.
So what's the 'take home' message?
Microsurgery in Male Infertility
If a patient has undergone vasectomy, and wants it reversed for some reason, excellent success rates can be provided microsurgically, at a center of excellence. With the rising divorce and remarriage rates in society worldwide, and an increase in geriatric sexuality, this operation is being performed more frequently than ever before. Also, people are more aware about the possibility of a surgical reversal, and thus come to the male infertility microsurgeon first, without going to other infertility centers where only TESA/ TESE (TEsticular Sperm Aspiration/ Extraction ) - ICSI (Intra-Cytoplasmic Sperm Injection) can be performed. A microsurgical vaso-vasostomy may also be required when the vas deferens is blocked due to other injury or disease, e.g. tuberculosis (TB), filariasis, etc.. These are common in tropical countries.
There are various techniques of microsurgical VVA available. These are outside the scope of a detailed discussion on a FAQ site such as www.varicocoele.com. Sometimes, the sperm conduction block is in the epididymis, not in the vas. The epididymis is the structure that connects the testis to the vas deferens. It is a long, convoluted tubule that nourishes the sperms during transit and allows for their maturation. To bypass such a block, the tubule of the epididymis is anastomosed (joined microsurgically) to the vas deferens using a variety of complex techniques.
Microsurgery of the epididymal tubule is generally conceded to be the most demanding and technically challenging of all microsurgical operations across all branches of surgery.
This is a procedure in which the male infertility microsurgeon uses the operating microscope to obtain sperms from the testis for an ICSI procedure. Multiple biopsies or aspirates may be obtained. Sometimes, the testis is incised open and a micro-dissection is performed before obtaining the best sperms from the best sperm-producing areas. These sperms are then transferred to a container and handed over to the reproductive biologist/ embryologist/ gynaecologist for further management.
Occasionally, vascular or vasculogenic impotence (ED), arterial or venous, may require to be treated microsurgically, e.g. in young men who have had pelvic fractures or bicycle injuries causing impotence.
|
| |||||||||||||||||||||||||||||||||||||
Home | News | Main Articles | Special Features | ||||||||||||||||||||||||||||||||||||||